Math Is Fun Forum
You are not logged in.
- Topics: Active | Unanswered
Pages: 1
#1 Today 17:03:56
- Jai Ganesh
- Administrator

- Registered: 2005-06-28
- Posts: 53,669
Ankylosing Spondylitis
Ankylosing Spondylitis
Gist
Spondylitis is a form of chronic, inflammatory arthritis primarily affecting the spine and sacroiliac joints, which can cause vertebra fusion and severe stiffness. Symptoms include chronic lower back/neck pain, stiffness that improves with activity, and fatigue. Treatment combines medications (NSAIDs, biologics), physical therapy, and exercise.
Spondylitis is primarily caused by an autoimmune response, where the body's immune system attacks healthy spine joints, strongly influenced by the HLA-B27 genetic marker. While the exact trigger is unknown, this chronic inflammation leads to stiffness and potential spinal fusion, often appearing in young adulthood.
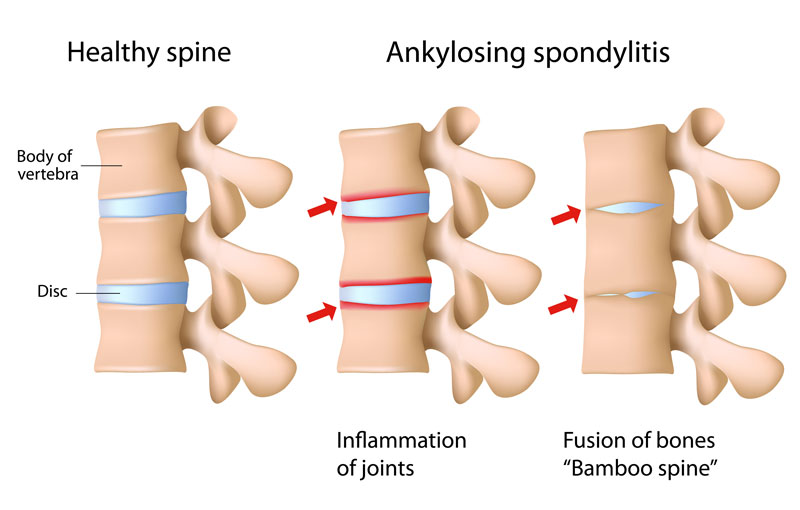
Ankylosing spondylitis (AS) is a type of arthritis that causes inflammation in certain parts of the spine. Ankylosing means stiff or rigid. Spondyl means spine. Itis refers to inflammation. The disease causes inflammation of the spine and large joints, resulting in stiffness and pain. The disease may damage the joint between the spine and the hipbone. This is called the sacroiliac joint. It may also cause bony bridges to form between vertebrae in the spine, fusing those bones. Bones in the chest may also fuse.
Summary
Spondylitis is an inflammation of the vertebrae. It is a form of spondylopathy. In many cases, spondylitis involves one or more vertebral joints, as well, which itself is called spondylarthritis.
Types
Pott disease is a tuberculous disease of the vertebrae marked by stiffness of the vertebral column, pain on motion, tenderness on pressure, prominence of certain vertebral spines, and occasionally abdominal pain, abscess formation, and paralysis.
Ankylosing spondylitis (AS) is a form of arthritis that primarily affects the spine, although other joints can become involved. It causes inflammation of the spinal joints (vertebrae) that can lead to severe, chronic pain and discomfort. In more advanced cases this inflammation can lead to ankylosis—new bone formation in the spine causing sections of the spine to fuse in a fixed, immobile position.
A combination of spondylitis and inflammation of the intervertebral disc space is termed a spondylodiscitis.
Details
Ankylosing spondylitis (AS) is a type of arthritis that affects the joints in your spine. It usually develops in your sacroiliac joints (where the bottom of your spine joins your pelvis). It causes typical arthritis symptoms like pain and stiffness, but it can also cause digestive symptoms, rashes and weight loss.
Overview:
What is ankylosing spondylitis?
Ankylosing spondylitis is a type of arthritis that affects joints in your spine. Healthcare providers sometimes call it axial spondylarthritis.
Ankylosing spondylitis (AS) also affects the joints where the base of your spine meets your pelvis (your sacroiliac joints). Your sacroiliac joints are the connection between your spine and pelvis. Specifically, they’re the place where the sacrum (the triangle-shaped last section of your spine) meets the ilium (the top and back part of your pelvis).
The sacroiliac joints are some of the biggest joints in your body, and you use them every time you move or shift your hips.
It’s less common, but ankylosing spondylitis can affect other joints, including your:
* Shoulders.
* Hips.
* Knees.
Ankylosing spondylitis causes pain, stiffness and gastrointestinal (GI) symptoms. Visit a healthcare provider if you’re experiencing lower back pain, especially if it’s getting worse or making it hard to do all your usual daily activities.
Symptoms and Causes:
What are ankylosing spondylitis symptoms?
Everyone with ankylosing spondylitis experiences a unique combination of symptoms. Lower back pain due to sacroiliitis (painful inflammation in your sacroiliac joints) is the most common AS symptom.
The pain can spread (radiate). You might experience other types of pain, including:
* Hip pain.
* Pain in your butt (buttocks).
* Neck pain.
* Abdominal (stomach) pain.
Other ankylosing spondylitis symptoms can include:
* Stiffness or trouble moving your hips and lower back (especially first thing in the morning or after you’ve been resting in one position for a long time).
* Fatigue (feeling tired all the time).
* Shortness of breath (dyspnea).
* Losing your appetite or having unexplained weight loss.
* Diarrhea.
* Skin rashes.
* Vision problems.
What causes ankylosing spondylitis?
Ankylosing spondylitis is an autoimmune disease. Autoimmune diseases happen when your immune system attacks your body instead of protecting it.
Experts aren’t certain what causes ankylosing spondylitis. Studies have found that specific genetic mutations are closely linked to having AS. Genetic mutations are changes to your DNA sequence that happen when your cells divide to make copies of themselves.
There are more than 60 mutated genes that might cause AS. One example is the human leukocyte antigen-B (HLA-B27) gene. More than 90% of white people who have AS also have a mutated HLA-B27 gene.
What are the risk factors?
Anyone can develop ankylosing spondylitis, but certain groups of people are more likely to have it, including:
* People younger than 40 (more than 80% of people with AS are diagnosed when they’re around 30).
* Males.
* People who have a close biological relative with AS (especially a biological parent).
People with certain health conditions are more likely to have ankylosing spondylitis, including:
* Crohn’s disease.
* Ulcerative colitis.
* Psoriasis.
What are the complications of ankylosing spondylitis?
People with ankylosing spondylitis have a higher risk of spinal fractures (broken bones in your spine).
Other complications can include:
* Fused vertebrae (bones in your spine joining together).
* Kyphosis (a forward curve in your spine).
* Osteoporosis.
* Eye and vision issues like uveitis or light sensitivity.
* Heart issues, including aortitis, arrhythmia and cardiomyopathy.
* Nerve damage.
Diagnosis and Tests:
How do providers diagnose ankylosing spondylitis?
A healthcare provider will diagnose ankylosing spondylitis with a physical exam. They’ll examine your body and discuss your symptoms. Tell your provider when you first noticed pain or other symptoms, including if any time of day or activity makes them worse.
You might need to visit a rheumatologist, a healthcare provider who specializes in treating arthritis and similar conditions.
What tests do healthcare providers use to diagnose ankylosing spondylitis?
There’s no one test that can confirm you have AS. Your provider might use a few tests to help diagnose it, including:
* Sacroiliac joint and spine X-rays to check for signs of arthritis.
* Magnetic resonance imaging (MRI), which can show more details than X-rays.
* Blood tests to check for the mutated HLA-B27 gene.
Management and Treatment:
How is ankylosing spondylitis treated?
Your healthcare provider will suggest treatments to manage your symptoms and reduce how much they affect your daily routine.
Common treatments for ankylosing spondylitis include:
* Exercise: Regular physical activity can reduce stiffness and stop AS from getting worse. Many people experience more severe pain when they’re inactive. A physical therapist can suggest specific stretches and exercises to help strengthen the muscles that support your back and spine.
* Nonsteroidal anti-inflammatory drugs (NSAIDs): Over-the-counter (OTC) NSAIDs, including ibuprofen and naproxen ease pain and inflammation. Talk to your provider before taking NSAIDs for more than 10 days in a row
* Biologic disease-modifying anti-rheumatic drugs (DMARDs): Biologic DMARDs are prescription medications that reduce inflammation and pain. They might also stop AS from getting worse.
* Corticosteroids: Corticosteroids are prescription anti-inflammatory medications. You might need cortisone shots (an injection of corticosteroids directly into your affected joints).
* Surgery: It’s rare to need surgery to treat AS. Your provider will usually only suggest it if you have severe symptoms that don’t get better after trying other treatments.
How soon will I feel better?
You should start feeling better soon after starting treatment. Your symptoms might not completely go away, but they should improve as you find treatments that work for you. Ask your provider when to expect improvements. Exercise and physical therapy are a gradual process, and medications take different amounts of time to take effect.
Outlook / Prognosis:
What can I expect if I have ankylosing spondylitis?
Ankylosing spondylitis is a chronic (long-term) condition. You should expect to manage your symptoms for a long time (maybe the rest of your life). Some people with AS have periods of remission where they have fewer, or milder, symptoms. Even if it’s been a while since you experienced symptoms, there’s always a chance they can come back.
There’s no cure for AS (or any other type of arthritis), but that doesn’t mean you have to live in pain. Talk to your provider about what you’re feeling. Tell them how much your symptoms impact your ability to do your favorite activities.
Living With:
How do I take care of myself?
In addition to following your AS treatment regimen, there are some steps you can take to reduce inflammation in your body and stress on your joints:
* Follow a diet and exercise plan that’s healthy for you.
* Limit how much alcohol you drink.
* Quit smoking.
When should I see my healthcare provider?
Visit your healthcare provider if you notice new symptoms, or if your symptoms get worse. Talk to your provider if it feels like your treatments aren’t managing your symptoms as well as they used to.
See a healthcare provider if you experience any of the following symptoms:
* Chest pain.
* Difficulty breathing.
* Vision problems.
* Severe back pain or other joint pain.
* Your spine feels unusually stiff or rigid.
* Unexplained weight loss.
What questions should I ask my healthcare provider?
Questions to ask your provider include:
* Do I have ankylosing spondylitis or another type of arthritis?
* Will I need genetic testing?
* Which treatments will manage my symptoms?
* Will I need physical therapy?
Additional Information:
Overview
Ankylosing spondylitis, also called axial spondyloarthritis, is a type of inflammatory disease that mainly affects the spine. Over time, the inflammation can cause some of the bones in the spine, called vertebrae, to fuse together. This fusing makes the spine less flexible and can lead to a hunched posture. If the joints in the chest are affected, it may become harder to take deep breaths.
Axial spondyloarthritis has two types. When the condition is found on X-ray, it is called ankylosing spondylitis, also known as axial spondyloarthritis. When the condition cannot be seen on X-ray but is found based on symptoms, blood tests and other imaging tests, such as an MRI, it is called nonradiographic axial spondyloarthritis.
Symptoms often begin in early adulthood. The condition also can cause inflammation in other parts of the body. This happens most often in the eyes, called uveitis.
There is no cure for ankylosing spondylitis, but treatments can lessen symptoms, manage pain and possibly slow down the progression of the disease.
Ankylosing spondylitis
As ankylosing spondylitis progresses, the body forms new bone in an effort to heal inflamed areas. The new bone gradually bridges the gaps between vertebrae and eventually fuses sections of vertebrae together. Fused vertebrae can flatten the natural curves of the spine, which leads to stiffness and a hunched posture.
Symptoms
Early symptoms of ankylosing spondylitis might include back pain and stiffness, especially in the lower back and hips. These symptoms may be worse in the morning or after periods of inactivity. Neck pain and fatigue also are common. Other symptoms include vision changes or eye pain, skin rashes and stomach pain.
Symptoms can come and go over time. Some people have periods of increased pain and stiffness, followed by times when symptoms improve or go away for a while.
The most commonly affected areas are:
* The joints between the base of the spine and the pelvis, called sacroiliac joints.
* The vertebrae in the lower back.
* The places where tendons and ligaments attach to bones, mainly in the spine or along the back of the heel.
* The cartilage between the ribs and the breastbone.
* The hip and shoulder joints.
When to see a doctor
See a healthcare professional if you have low back or buttock pain that comes on slowly. Also see a healthcare professional if the pain feels worse in the morning or awakens you from your sleep at night, especially if this pain improves with exercise and worsens with rest. You also should seek care from an eye specialist right away if you develop a red, painful eye, light sensitivity or blurry vision since these can be signs of inflammation in the eye.
Causes
The exact cause of ankylosing spondylitis isn't known, but genetic factors seem to be involved. People who have a gene called HLA-B27 are at a greatly increased risk of developing ankylosing spondylitis. However, only some people with the gene develop the condition and not everyone with ankylosing spondylitis has this gene.
Risk factors
Risk factors for ankylosing spondylitis include:
* Younger age. The disease usually starts in late adolescence or early adulthood.
* Genetics. Most people who have ankylosing spondylitis have the HLA-B27 gene. But many people who have this gene never develop ankylosing spondylitis.
Complications
In serious cases of ankylosing spondylitis, the body tries to heal the long-term inflammation by forming new bone. Over time, this new bone bridges the gaps between vertebrae and causes them to fuse together. The fused parts of the spine become stiff and less flexible. If the joints in the chest around the rib cage also become stiff, the stiffness can limit how much the lungs can expand and make deep breathing more difficult.
Other possible complications include:
* Eye inflammation, called uveitis. Uveitis is one of the most common complications of ankylosing spondylitis. It can cause sudden eye pain, redness, light sensitivity and blurry vision. See your healthcare professional right away if you develop these symptoms.
* Compression fractures. When the bones in the spine weaken, they can press together and make a hunched posture worse. Vertebral fractures also can press on and possibly damage the spinal cord and nerves.
* Heart issues. Ankylosing spondylitis can cause issues with the aorta. The aorta is the largest artery in the body. When the aorta gets inflamed, it can swell and change the shape of the aortic valve in the heart. This makes the valve leak, and it can't work as well. This is called aortic regurgitation. This inflammation also increases the overall risk of heart disease.
It appears to me that if one wants to make progress in mathematics, one should study the masters and not the pupils. - Niels Henrik Abel.
Nothing is better than reading and gaining more and more knowledge - Stephen William Hawking.
Offline
Pages: 1